Lost in the Fog of Caregiving
By: Geri Lynn Baumblatt, MA
Quick poll: Do you help a partner, an aging relative, friend, adult sibling, or ill or disabled child with things like:
-
Medical appointments or medications
-
Meals, bills, or insurance
-
Care coordination
-
Hands-on care
If you’re like 1 in 4 people in the U.S., you said yes.1 In fact, many people (about 25% of caregivers) even care for more than one adult.2
Why Caregiving Is Often Overlooked
However, we usually think of ourselves as daughters, sons, partners, or friends — not as informal/family caregivers or care partners. And both are true. But, over time — or in the blink of an eye —caregiving can become intense, overwhelming, and socially isolating. According to the new NAC report, on average, caregivers spend 27 hours per week providing care; and 24% provide 40 or more hours a week. 1
So, while failure to self-identify may not sound serious - caregivers often don’t get support or connect with resources early on. Then, suddenly they’re in over their heads.
The Hidden Health Impact
Caregiving is a social determinant of health. It often impacts their health and wellbeing. It’s not just serious lack of sleep, anxiety and depression, and trouble getting regular exercise — about 54% say they have no time to tend to their own medical needs. 3 They have:
-
Higher risk for strokes, heart attacks, and injuries
-
Greater reliance on alcohol, nicotine, or sleep medication
People often hit a point where they need to cut back on work, go part time or quit, creating serious financial straits, more stress -- and loss of employee-sponsored health insurance. And this is the person sitting next to the patient.
So, when people don’t recognize the activities they’re doing as caregiving, they’re kind of lost in the fog. This is usually a blind spot in our SDoH screening, in our medical records (there’s often not even a field to capture who a patient’s caregivers are), and in our conversations.
How might we help people recognize they’re caregiving, the long-term challenges and impacts it usually has on people — and better connect them with resources and support?
Clinicians, social workers, and other staff can start by simply asking patients who helps them and who they help care for, and what they do. When care teams get an awareness of this, it can inform whether the patient has any care partners, if they themselves are caring for others with more serious needs, and how that’s affecting their health. It can also help the someone recognize they’re a caregiver -- and if what they’re care role is becoming more intense.
Tools and Programs That Help
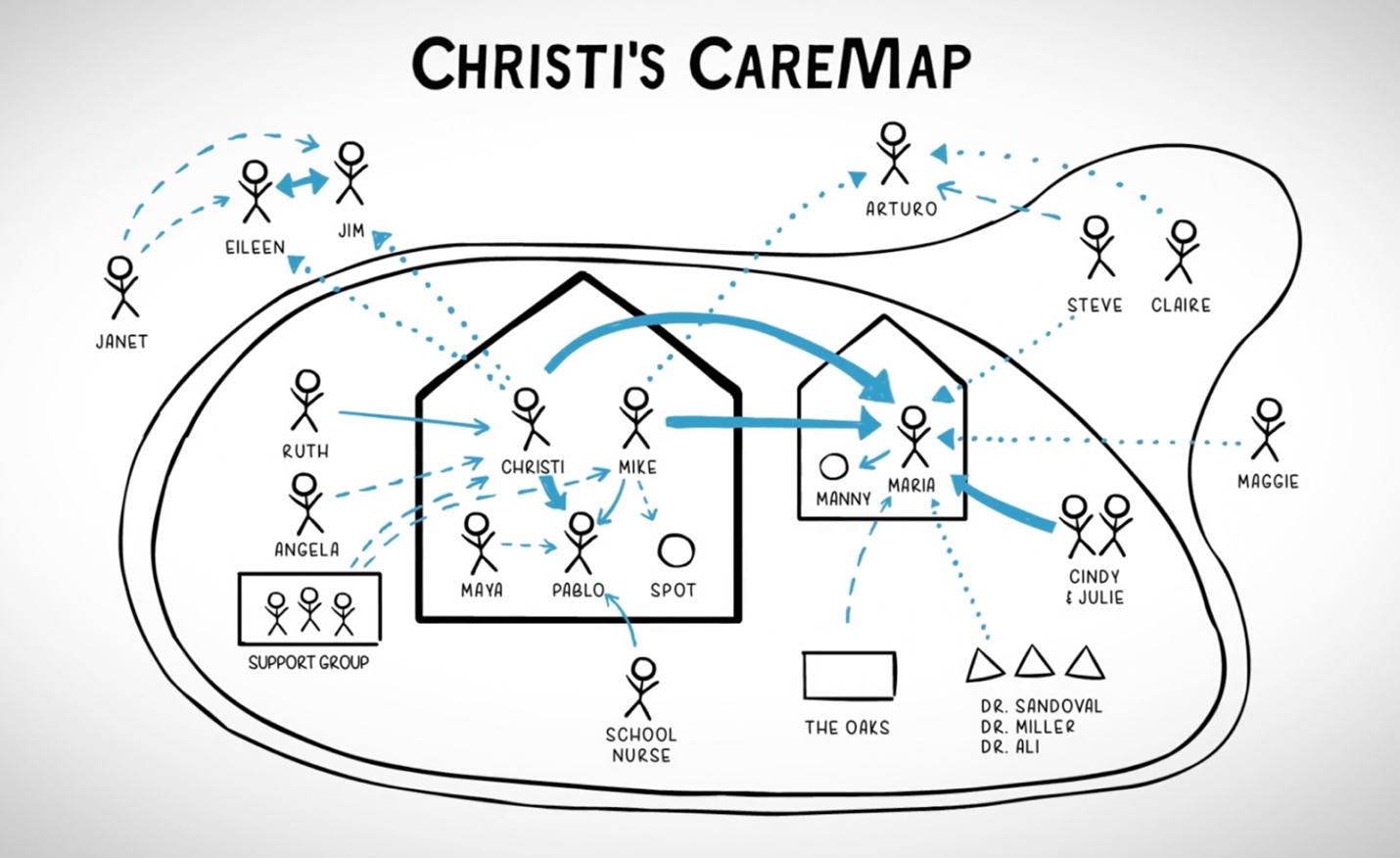
Another great tool is Atlas CareMaps.4 It’s a way to draw a quick map of a care ecosystem to understand the current state, plan for possible problems, and identify missing people and services. I recommend trying it yourself. Even as someone who talks about caregiving a lot, I gleaned key insights from doing it. Plus, it creates an artifact you can share with the care team and update.
A more serious event, like a hospitalization, is often when many people become or start to realize they’ll need to spend more time caregiving. This is also an opportunity to help people realize that caregiving usually extends beyond the immediate recovery from an injury or surgery. A program called the Ken Hamilton Caregiver Center5 has now been replicated at many hospitals to help reach out to caregivers at the hospital and support them after they leave.
Another way to help and to identify caregivers is to suggest people add family care partners to their portal/MyChart through shared (proxy) access. In fact, if you haven’t done this yourself, it’s much better than logging into someone else’s portal as them. And it’s good to see how easy or hard this is to do this in your system’s portal. The Coalition for Care Partners6 created shared access toolkits for patients/caregivers and clinicians and systems.
Helping people identify as caregivers/care partners needs to be integrated into our health systems. Too often, caregivers become second-order patients.
How are there opportunities in your work and organization to help with this? Please share anything you do or any ideas you have here.
Citations
- National Alliance for Caregiving & AARP. Caregiving in the US 2025 Report
- Caregiving in the U.S. 2020 Report. AARP
- For the Benefit of All: Voya Cares Whitepaper, 2019
- Atlas of Caregiving: Atlas Care Maps, 2020
- Ken Hamilton Caregiver Center
- Care Partners and Health IT, Coalition for Care Partners
About the Author:
Geri Lynn Baumblatt, MA, has worked in patient engagement, education, shared decision making, care transitions, informed consent, design thinking, and health technology, and outcomes research for over 25 years. She oversaw the creation of Emmi’s multimedia patient education library, was the multimedia expert on AHRQ’s PEMAT, served on PCORI’s Patient Engagement Advisor Panel, and continues to serve on the Leadership Board of the Journal of Patient Experience. She consults on patient/family engagement, caregiving, like OpenNotes, UVA, Baylor, Tufts, and the VA. She oversees patient education for the Rush University Medical Center and is an advocate for patients and informal/family caregivers.
#IHABlog
#InformalCaregivers
#OlderPatients